Connect with us:
Blog
Items filtered by date: December 2019
Don't Skip Diabetic Foot Exams. Here's What's at Stake
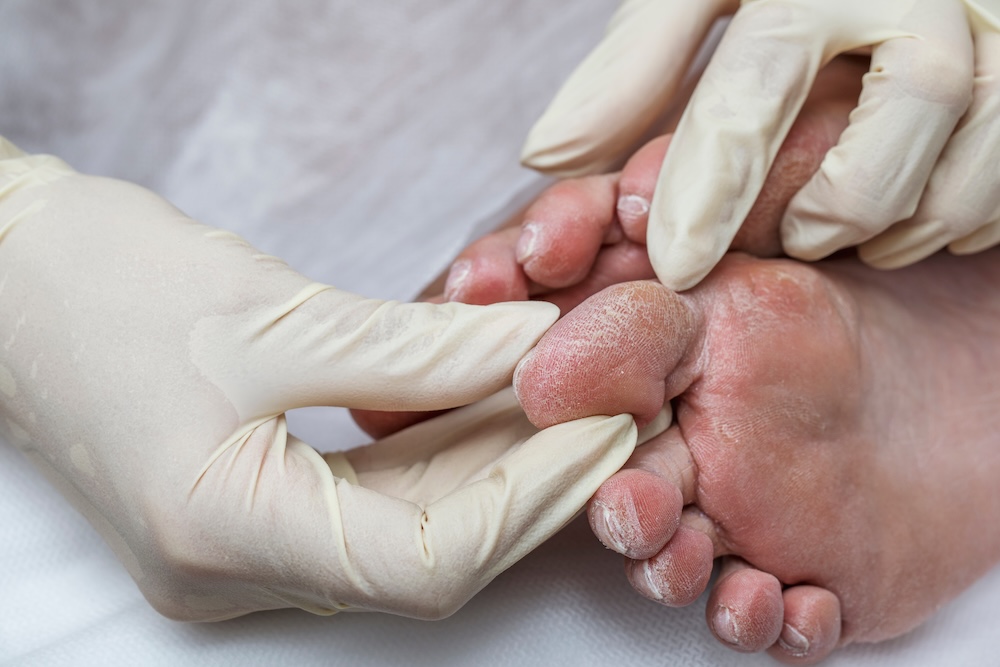 For diabetic patients, a routine diabetic foot exam does far more than check for obvious injuries. It catches the small things — a blister, a callus, an ingrown nail — before they become infections or worse. What heals quickly for most patients can spiral into a serious complication for someone managing diabetes. Understanding what a podiatrist for diabetic foot care looks for, and why, helps you stay ahead of problems.
For diabetic patients, a routine diabetic foot exam does far more than check for obvious injuries. It catches the small things — a blister, a callus, an ingrown nail — before they become infections or worse. What heals quickly for most patients can spiral into a serious complication for someone managing diabetes. Understanding what a podiatrist for diabetic foot care looks for, and why, helps you stay ahead of problems.
The American Diabetes Association recommends a complete foot examination for diabetes patients at least once a year. You may benefit from more frequent visits if you’re dealing with diabetic neuropathy or circulation concerns. These regular check-ins help patients monitor long-term foot concerns and address smaller issues that can quickly become dangerous for people with diabetes.
Dr. Patrick Nunan, a podiatrist at Physicians Footcare, puts it plainly: "It is much easier to keep you out of trouble than to try and fix you if you get in trouble."
Why Diabetes Makes Minor Foot Problems More Dangerous
Diabetes affects the feet through two primary mechanisms: nerve damage and reduced blood flow. Diabetic neuropathy — specifically, peripheral neuropathy — dulls sensation in the feet over time. A small cut or blister may cause no pain at all, which means you may not notice it until the problem has already advanced.
At the same time, poor circulation caused by blood vessel damage slows healing and limits the body's ability to fight infection. People with diabetes face a significantly higher risk of developing diabetic foot ulcers — open sores that can become infected and, in serious cases, lead to amputation. Controlling blood pressure and blood sugar levels are both essential to slowing that progression.
Common Foot Problems That Can Become Serious in Diabetes Patients Without a Diabetic Foot Exam
Several common foot conditions that cause mild discomfort in most people become serious threats for diabetic patients. During a foot examination for diabetes, your podiatrist carefully assesses each of the following.
Blisters: A Minor Nuisance That Can Turn Into a Major Problem
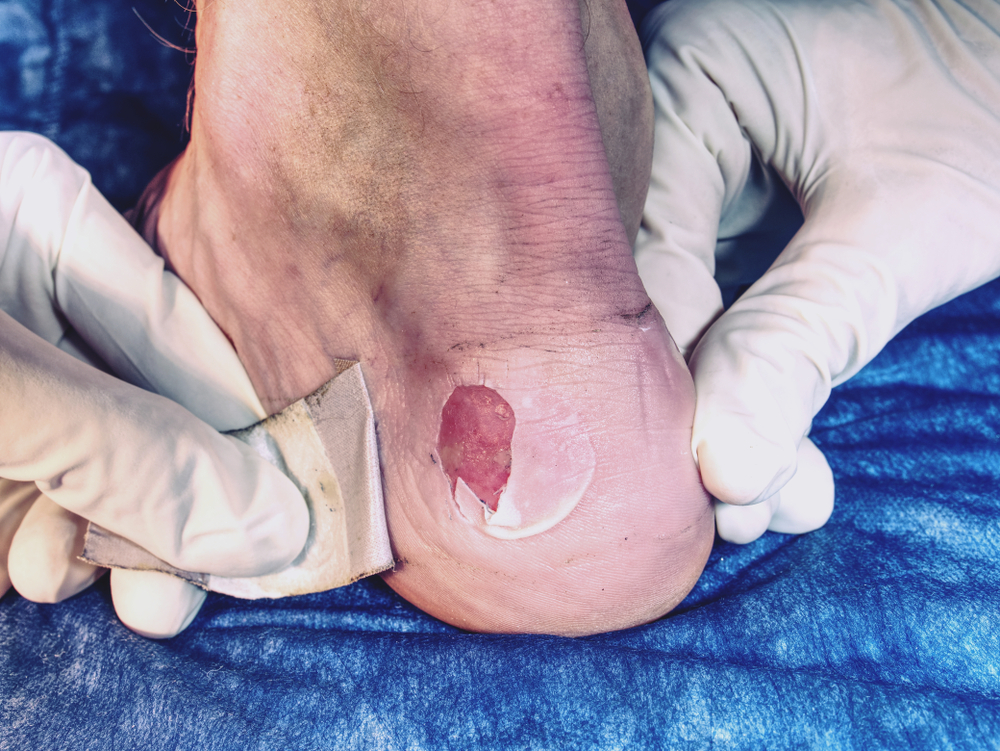 Blisters on the feet form when friction or pressure creates fluid-filled pockets under the skin. Because diabetes can reduce sensation in the feet, a blister may rupture and become infected before you notice it. Even a small, seemingly harmless blister can progress into an open wound without proper attention.
Blisters on the feet form when friction or pressure creates fluid-filled pockets under the skin. Because diabetes can reduce sensation in the feet, a blister may rupture and become infected before you notice it. Even a small, seemingly harmless blister can progress into an open wound without proper attention.
What Your Podiatrist Checks: Skin integrity, signs of infection, circulation in surrounding tissue, and whether footwear is contributing to the friction.
What to Expect From Treatment: A podiatrist for diabetic feet will typically leave small intact blisters to heal on their own, draining and dressing larger ones in a sterile clinical setting. Footwear adjustments or cushioned padding often prevent recurrence.
Minor Cuts and Wounds: Why They Demand an Immediate Foot Examination for Diabetes Patients

A minor cut is rarely cause for concern in most people. When diabetes is involved, even a small wound can become a high-stakes situation. Reduced sensation means injuries often go undetected, and slower healing creates a longer window for bacteria to take hold and infection to set in.
What Your Podiatrist Checks: Wound depth, active signs of infection, surrounding tissue health, and blood flow to the affected area.
What to Expect From Treatment: Diabetic foot pain treatment for open wounds typically involves thorough cleaning, debridement if needed, and antibiotics for any active infection, along with close follow-up visits to monitor the healing process.
Corns and Calluses: How Pressure Buildup Becomes a Danger Zone Without a Diabetic Foot Exam
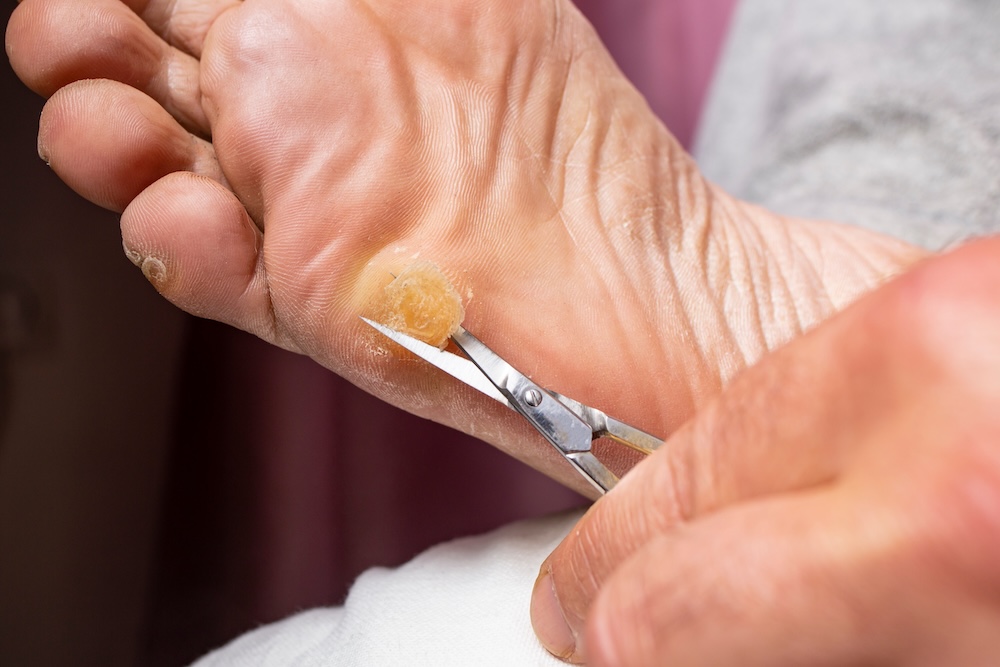 Corns and calluses develop from repeated pressure or friction on the skin. In diabetic patients, thick skin buildup creates concentrated pressure points that can break down into open sores over time. Reduced sensation often means the buildup advances faster than you might think.
Corns and calluses develop from repeated pressure or friction on the skin. In diabetic patients, thick skin buildup creates concentrated pressure points that can break down into open sores over time. Reduced sensation often means the buildup advances faster than you might think.
What Your Podiatrist Checks: Callus thickness and location, whether ulceration is forming, and whether gait mechanics or footwear are the main cause.
What to Expect From Treatment: Diabetic foot pain treatment for corns and calluses involves safe professional removal by a foot specialist. Taking care of your feet at home and avoiding sharp self-treatment tools between visits reduces the risk of accidental injury.
Ingrown Toenails: A Small Nail Problem With Serious Infection Risk
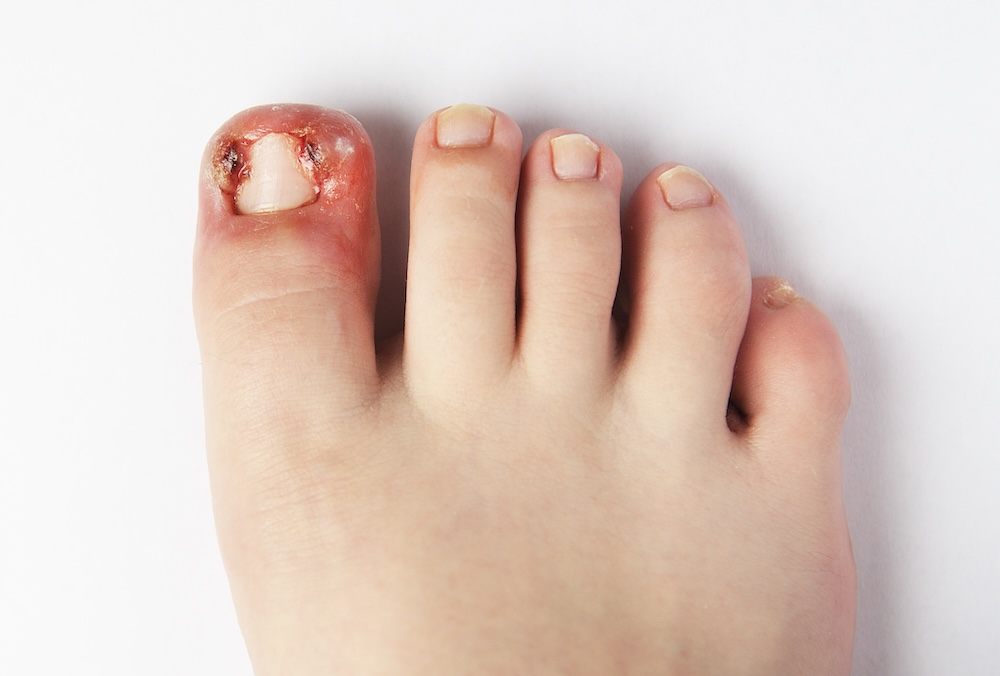 An ingrown toenail occurs when the nail edge grows into the surrounding skin. In most people, this produces localized pain and mild swelling. In diabetic patients, even a minor ingrown nail can become a gateway for bacteria, with infection spreading into the surrounding tissue quickly and sometimes without obvious warning signs.
An ingrown toenail occurs when the nail edge grows into the surrounding skin. In most people, this produces localized pain and mild swelling. In diabetic patients, even a minor ingrown nail can become a gateway for bacteria, with infection spreading into the surrounding tissue quickly and sometimes without obvious warning signs.
What Your Podiatrist Checks: Redness, swelling, drainage, and whether infection has spread beyond the nail border.
What to Expect From Treatment: A podiatrist for diabetic foot care may lift or partially remove the nail under local anesthesia, followed by careful dressing and close monitoring. Diabetic foot pain treatment for ingrown toenails often includes antibiotics when infection is present.
Fungal Infections: Why Diabetic Patients Can't Afford to Ignore Them
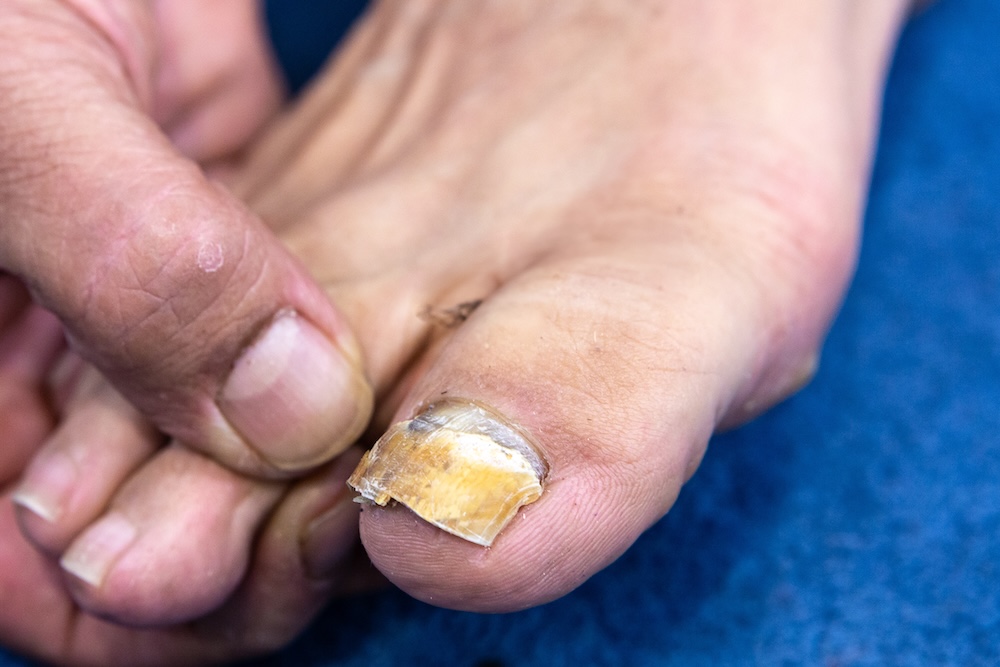 Fungal infections, like athlete's foot and fungal toenails, thrive in warm, moist spaces. For diabetics, these infections create entry points in the skin that bacteria can exploit. Reduced immune response and circulation make fungal infections harder to clear and more likely to spread.
Fungal infections, like athlete's foot and fungal toenails, thrive in warm, moist spaces. For diabetics, these infections create entry points in the skin that bacteria can exploit. Reduced immune response and circulation make fungal infections harder to clear and more likely to spread.
What Your Podiatrist Checks: Skin condition between the toes, nail discoloration or thickening, and skin breakdown in or near affected areas.
What to Expect From Treatment: Treatment during a foot examination for diabetes typically includes prescription topical or oral antifungal medications. Your podiatrist will also recommend specific footwear hygiene and moisture management practices to reduce the chance of recurrence.
Daily Habits That Help Prevent Diabetic Foot Complications
Taking steps to protect your feet every day is one of the most effective ways to prevent diabetic foot complications before they require medical intervention. As Dr. Kevin Uren of Physicians Footcare reminds his patients: "Diabetics out there: Take care of your feet, and they will take care of you."
Building these daily foot care habits into your routine makes a measurable difference:
- Check Your Feet Daily. Inspect the entire foot — top, bottom, sides, and between the toes. Look for cuts, blisters, redness, swelling, or any skin changes that weren't there before. Use a mirror if you have trouble seeing the bottom of your feet.
- Wear Proper Footwear. Well-fitted shoes with adequate cushioning reduce the friction and pressure that lead to blisters, corns, and calluses. Avoid going barefoot, even indoors.
- Keep Feet Clean and Moisturized. Wash and dry your feet thoroughly each day. Apply moisturizer to prevent dry, cracking skin, but skip the areas between your toes to avoid trapping moisture where fungus thrives.
- Manage Your Blood Sugar Consistently. Elevated blood sugar accelerates damage to nerves and blood vessels throughout the body, and your feet bear the consequences more than most areas.
- Schedule Regular Diabetic Foot Exams. A podiatrist for diabetic foot care catches the small problems before they escalate into serious ones. Those with neuropathy or circulation concerns should schedule a foot examination for diabetes more than once a year.
When to See a Podiatrist for Diabetic Foot Problems
Knowing when to call a podiatrist for a diabetic foot exam is a critical part of managing diabetes effectively. Seek professional help right away if you notice a wound that isn't healing, worsening redness or swelling, discharge or odor coming from a cut or blister, nail changes, or numbness that spreads. Don't wait to see if something resolves on its own. With diabetes, waiting typically makes things worse. A foot examination for diabetes is the best way to prevent serious issues from developing.
For expert diabetic foot care, the podiatrists at Physicians Footcare bring both clinical expertise and genuine personal commitment to every patient they see. Dr. Keyoka Smith, one of Physicians Footcare's podiatrists with a special focus in diabetic foot care, speaks to that mission directly: "Inspired by my grandparents' journey with diabetes, I've dedicated my career to helping patients heal, prevent complications, and advocate for themselves in partnership with their doctors."
That patient-first approach is reflected across Physicians Footcare's seventeen locations in South Carolina and Georgia. Our team of podiatrists provides thorough foot examinations for diabetes care, diabetic foot pain treatment, and ongoing support for your foot health. Whether managing a chronic condition or simply due for a diabetic foot exam, our podiatrists will get you back on your feet and build a care plan around your specific needs.
Schedule your appointment today or call (833) PFC-FOOT to get started.
Physicians Footcare Welcomes Dr. Steven Silvestro
 Florence, SC- Physicians Footcare, the Southeast’s premier podiatric practice is pleased to announce that Dr. Silvestro will be joining our team. He will begin treating patients in our Florence office in April.
Florence, SC- Physicians Footcare, the Southeast’s premier podiatric practice is pleased to announce that Dr. Silvestro will be joining our team. He will begin treating patients in our Florence office in April.
Dr. Silvestro completed his residency at INVOA Fairfax Medical Campus in Falls Church, VA. He is a member of the American Board of Podiatric Medicine and the American Board of Foot and Ankle Surgery. He brings extensive knowledge in the areas of biomechanics, wound care and reconstructive surgery.
“I look forward to joining Physicians Footcare and sharing my passion for foot and ankle health to improve patient mobility and quality of life,” says Silvestro.
"Physicians Footcare is thrilled to announce the addition of Dr. Silvestro to our Florence team. As the 2022 valedictorian of New York College of Podiatric Medicine, he brings an unparalleled level of academic excellence and modern clinical insight to our practice,” said Dr. Ray, CEO Physicians Footcare. He views foot & ankle health as the literal foundation of a patient’s well-being, and his superior training ensures that our Florence patients are in the most capable hands.”
To schedule an appointment with Dr. Silvestro, contact our Florence Office at (843) 665-4567. To learn more about Physicians Footcare and the array of healthcare services we provide, visit www.physiciansfootcare.com.
About Physicians Footcare
Physicians Footcare is one of the largest podiatric practices in the southeast and the nation. It is the Southeast’s premier podiatry practice, independently and privately owned. Since opening our first location in 2006, we have grown to locations in South Carolina, Georgia, and New York. Our mission is simple-To Be the Best Medical Practice.
Sprained Ankle vs. Broken Ankle: How to Tell the Difference
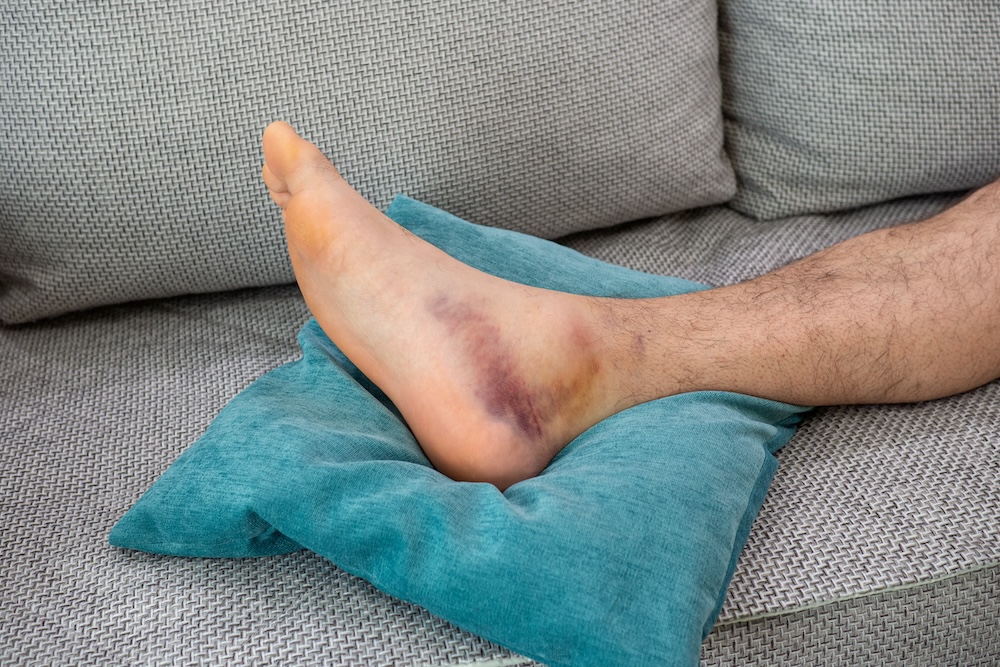 You roll your ankle, feel sudden pain, and then the question hits fast: Is it a sprain or a break? When symptoms like swelling, bruising, or difficulty walking appear, it can be hard to tell the difference between a sprained ankle vs. a broken ankle.
You roll your ankle, feel sudden pain, and then the question hits fast: Is it a sprain or a break? When symptoms like swelling, bruising, or difficulty walking appear, it can be hard to tell the difference between a sprained ankle vs. a broken ankle.
Understanding how to tell if an ankle is broken or sprained is important because the right treatment depends on the type of injury. While some sprains improve with rest and support, a fracture may require more advanced care. Ignoring the difference can lead to longer recovery times or complications.
In this guide, we’ll break down the key signs of a broken or sprained ankle, compare symptoms of a sprained ankle vs. a broken ankle, and explain what to do if you’ve rolled your ankle and aren’t sure what’s wrong. Let’s take a closer look at how to tell what your ankle injury really means.
What Is an Ankle Sprain?
An ankle sprain happens when the ligaments that support your ankle are stretched or torn. Ligaments are strong bands of tissue that connect bones and help stabilize your joints, so when they get injured, it can cause pain and affect your ability to walk or move comfortably.
Sprains can range from mild overstretching to more severe tears and ligament damage, so it’s important to recognize the signs early.
Common Causes of Sprained Ankles
Ankle sprains occur during sports, exercise, or even routine daily movement when the foot twists inward or rolls awkwardly. If you have a rolled ankle that is broken or sprained, it can be difficult to tell which injury it is at first. In many cases, though, a rolled ankle causes damage to the ligaments that support the joint, which means the injury is a sprain.
Common causes of an ankle sprain include:
- Rolling or twisting your ankle while walking on an uneven surface
- Landing awkwardly after a jump or fall
- Sudden changes in direction while running or playing sports
Symptoms of a Sprained Ankle
Symptoms can vary depending on the severity of the sprain, but common signs include:
- Pain around the ankle, especially when bearing weight
- Swelling and tenderness
- Bruising or discoloration
- Limited range of motion or difficulty moving the joint
These sprained ankle symptoms can sometimes overlap with broken ankle symptoms. That’s why a medical evaluation from a podiatrist is the best way to determine the nature of your injury and the best treatment option for you.
Ankle Sprain Diagnosis and Treatment
Even if you think you only have a mild sprain, it’s important to get a professional evaluation. A doctor may perform a physical exam and sometimes order an X-ray or MRI to rule out a fracture or more serious injury.
Treatment usually focuses on relieving pain, reducing swelling, protecting the joint, and helping the ankle heal correctly. Common approaches include:
- RICE method: Rest, ice, compression, and elevation can help reduce pain and swelling in the early stages.
- Bracing or support: An ankle brace or walking boot can stabilize the joint and limit further strain.
- Physical therapy: Guided exercises help restore strength, flexibility, balance, and range of motion.
- Pain relievers: Over-the-counter medications may help keep you comfortable during recovery.
With proper care, most ankle sprains heal well. However, returning to activity too soon or disregarding sprained ankle recovery guidelines can raise the risk of ongoing instability or re-injury.
What Is a Broken Ankle?
A broken ankle, also called an ankle fracture, occurs when one or more of the bones that form the ankle joint — the tibia, fibula, or talus — crack or break. Unlike a sprain, which affects the ligaments, a broken ankle involves the bones themselves and requires more intensive treatment to heal properly.
Common Causes of Broken Ankles
Broken ankles most often happen during high-impact activities or accidents, such as:
- Falling from a height or tripping on stairs
- Sports-related injuries involving sudden twists or collisions
- Car accidents or other high-impact trauma
Symptoms of an Ankle Break
An ankle fracture tends to be more obvious and severe than a sprain. Common signs include:
- Sharp or intense pain
- Swelling and bruising around the ankle
- Visible deformity or misalignment of the ankle or foot
- Inability to bear weight, walk, or put pressure on the affected ankle
These symptoms are often more severe when comparing sprained ankle vs. broken ankle symptoms, although both conditions may initially look similar.
Broken Ankle Diagnosis and Treatment
A broken ankle always needs professional evaluation. A podiatrist will examine the injured ankle and usually order imaging, most often an X-ray, to confirm the fracture and understand how severe it is. In some cases, additional imaging such as an MRI may be needed.
Broken ankle treatment depends on which bone is broken, whether the fracture is stable, and whether the bones have shifted out of place. Common treatment options include:
- Casting or splinting: A cast or splint helps keep the ankle bones in proper alignment while they heal.
- Surgery: More severe fractures may require surgery to reposition the bones and stabilize them with plates, screws, or other hardware.
- Physical therapy: Once the bone has healed enough, rehabilitation can help restore strength, mobility, and normal ankle function.
Prompt treatment is important. Unlike a sprained ankle, an untreated fracture can heal improperly and lead to ongoing pain, instability, or arthritis.
Sprained Ankle vs. Broken Ankle: Key Differences
Because sprains and fractures share many symptoms, like pain, swelling, and bruising, it can sometimes be difficult to tell if your ankle is broken or sprained. However, there are a few key differences that may help you better understand what type of injury you might be dealing with.
- Pain intensity and location: An ankle sprain usually causes pain near the ligaments that support the joint. It may be more localized. A broken ankle often causes sharper, more severe pain directly over the affected bone.
- Ability to bear weight: Many people with a mild ankle sprain can still put some weight on the injured foot, even if it’s uncomfortable. It is extremely difficult, or impossible, to stand or walk on a broken ankle.
- Swelling and bruising patterns: Both injuries can cause swelling and bruising, but the timing and severity for a sprained ankle vs. a broken ankle can differ. Sprains may cause moderate swelling that builds slowly, while fractures often cause more swelling that starts soon after injury.
- Visible deformity: In some cases, a broken ankle can cause the affected foot or ankle to look misaligned or visibly out of place. This can be a strong sign that the bones are fractured and require immediate medical attention.
- Response to rest and elevation: Sprains sometimes begin to improve with basic at-home care such as rest, ice, compression, and elevation (RICE). A fracture, however, frequently fails to get better with these measures. It can still trigger intense pain and restrict movement.
While these differences can offer helpful clues, it’s not always easy to tell if an ankle is broken or sprained without a professional diagnosis. If you’re unsure about your injury, it’s best to seek medical care with a podiatrist you trust.
How to Prevent Broken or Sprained Ankles
A few simple steps can help protect your ankles and reduce the risk of injury. Follow these practical tips:
- Strengthen and stretch your ankles: Regular exercises that improve ankle strength and flexibility can help prevent sprains and other injuries. Simple stretches, balance exercises, and light resistance training are great ways to keep your joints stable.
- Be cautious on uneven surfaces: Pay attention to where you step, especially on trails, stairs, or slippery surfaces. Taking your time and staying mindful of your footing can help prevent twists and falls.
- Wear the right footwear: Supportive shoes that fit well, custom orthotics, and are appropriate for your activity can make a big difference, especially during sports, workouts, or long walks. As Physicians Footcare certified pedorthist Natalie McCoy says, “When it comes to your footwear, being properly measured and knowing what general size is appropriate for your foot and its unique needs is imperative to good foot health and daily comfort.”
By incorporating these habits into your routine, you can help keep your ankles strong and reduce the likelihood of injuries.
Broken or Sprained Ankle? Here’s What to Do
Understanding the difference between a sprained ankle vs. a broken ankle is important for proper healing and preventing long-term problems. While some injuries may seem minor, it’s not always easy to tell the difference on your own. If you’re unsure how serious your ankle pain, swelling, or walking trouble is, a podiatrist can offer a professional diagnosis and get you on the right track toward recovery.
At Physicians Footcare, our experienced team of podiatrists and certified pedorthists can assess your ankle, provide an accurate diagnosis, and recommend the right treatment to help you recover safely. As Dr. Patrick Nunan, podiatrist at Physicians Footcare, says, "Our goal is to diagnose your problem, treat the problem, and return you to the activities that you enjoy."
Schedule a podiatry appointment today to make sure your ankle gets the care it needs.
Physicians Footcare Welcomes Dr. Dolores Farrer

Dr. Farrer brings decades of podiatric experience to the Midlands, specializing in wound care. She is licensed in both South Carolina and Georgia. Additionally, she has been certified by the American Board of Wound Management for over 20 years and currently serves as the secretary of the Board of Directors for the Association for the Advancement of Wound Care.
"I am excited to join Physicians Footcare as the newest chapter in my 30-year career. My goal has always been to use my extensive clinical experience combined with the latest evidence-based treatments to provide quality footcare. By maintaining active professional memberships and leadership roles, I will ensure PFC patients benefit from the most advanced standards of care,” says Farrer.
“We are thrilled to welcome Dr. Dolores Farrer to our practice, said Dr. Ray, CEO of Physicians Footcare. After more than three decades in podiatric care, she has extensive knowledge in treating advanced conditions and expertise in improving outcomes for patients with hard-to-heal wounds. We look forward to her providing unparalleled service to the Columbia community.”
To schedule an appointment with Dr. Farrer, contact our Cayce Office at (803) 796-0616. To learn more about Physicians Footcare and the array of healthcare services we provide, visit www.physiciansfootcare.com.
About Physicians Footcare
Physicians Footcare is one of the largest podiatric practices in the Southeast and nationwide. It is the Southeast’s premier podiatry practice, independently and privately owned. Since opening our first location in 2006, we have grown to locations in South Carolina, Georgia, and New York. Our mission is simple: to be the best medical practice.
What Causes Swollen Feet? Common vs. Serious Causes
S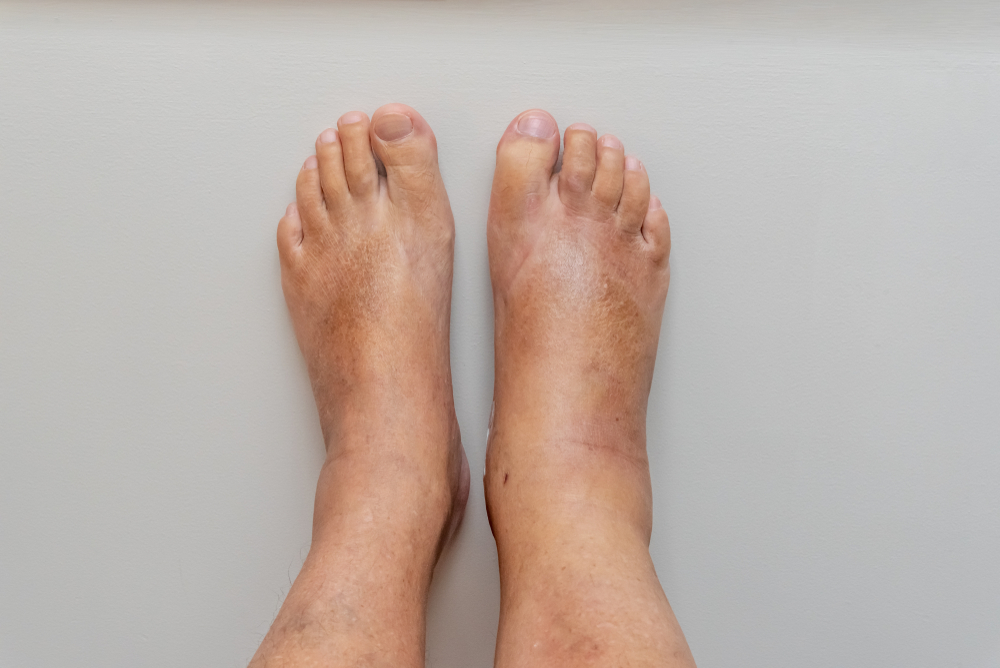 wollen feet can be caused by a wide range of factors, and while some are harmless and temporary, others may signal a more serious underlying health concern. Medically known as edema, this swelling occurs when excess fluid accumulates in the tissues, typically affecting the feet and ankles. Understanding what causes swollen feet is essential for knowing when swelling is simply an inconvenience and when swollen feet may be dangerous and require medical attention.
wollen feet can be caused by a wide range of factors, and while some are harmless and temporary, others may signal a more serious underlying health concern. Medically known as edema, this swelling occurs when excess fluid accumulates in the tissues, typically affecting the feet and ankles. Understanding what causes swollen feet is essential for knowing when swelling is simply an inconvenience and when swollen feet may be dangerous and require medical attention.
In many situations, swelling is linked to everyday factors that do not require a doctor’s visit. However, swollen feet can sometimes signal more serious conditions affecting circulation, joints, bones, or overall health. Learning to recognize the difference can help you determine when to worry about swollen feet and when simple at-home care is enough.
Causes of Swollen Feet
Swollen feet are often caused by temporary, non-podiatric factors and do not require immediate concern or medical attention. Pregnancy is a common cause due to increased fluid retention and pressure on the lower extremities. Certain medications, such as blood pressure medications, hormones, or anti-inflammatory drugs, are also common causes of swollen feet. Diet plays a role as well; consuming high-sodium foods may cause the body to retain excess fluid, resulting in swelling in the feet and ankles.
Lifestyle factors are another group of possible causes for swollen feet. Wearing tight socks or shoes, sitting or standing for long periods of time, and carrying excess body weight can all affect circulation and lead to fluid buildup. Mild allergic reactions, minor infections, and the natural aging process may also cause occasional swelling. In most cases, this swelling caused by less serious factors improves with movement, elevation, hydration, or dietary changes. However, swelling that persists or worsens should always be evaluated by a healthcare provider.
Swelling from Foot Fractures
Unlike mild or temporary swelling, swelling caused by a foot fracture is a sign of injury and requires medical attention. When a bone breaks, the body responds with inflammation, leading to noticeable swelling (edema) around the injured area.
In addition to swelling, common symptoms include:
- Pain that worsens with movement or weight-bearing
- Bruising
- Difficulty walking
- Tight and tender foot
- In some cases, pain is focused in one specific area
Most foot fractures take 6–8 weeks to heal with proper treatment. Swelling usually improves over time but may linger even after the bone heals. Rest, elevation, and following medical guidance are key to recovery.
Swelling from Sprains
Swelling from a sprain occurs when ligaments are stretched or torn, often due to twisting or rolling the foot or ankle. This inflammation is the body’s natural response to injury and can range from mild to severe depending on the extent of the damage.
In addition to swelling, common symptoms include:
- Pain
- Bruising
- Tenderness, especially when moving or bearing weight
- The area feels unstable or weak
Mild sprains may heal within a few weeks, while more severe sprains can take 6–8 weeks or longer. Rest, ice, compression, and elevation (RICE) are commonly used to manage swelling and support recovery.
Swelling from Arthritis
Arthritis-related swelling is caused by inflammation within the joints of the foot or ankle. It often develops gradually and may worsen over time, especially with activity.
In addition to joint swelling, symptoms include:
- Stiffness
- Pain
- Reduced range of motion
Swelling may be more noticeable in the morning or after long periods of movement.
Arthritis is a chronic condition, so swelling may come and go rather than fully resolve. Management typically focuses on reducing inflammation and pain through lifestyle changes, supportive footwear, and medical treatment.
Swelling from Tendonitis
Tendonitis occurs when tendons in the foot become irritated or inflamed due to overuse or repetitive stress. Swelling is usually localized along the affected tendon.
In addition to swelling, symptoms include:
- Tenderness
- Pain that worsens with movement or activity
- The area may feel warm or stiff, especially after rest
With proper care, tendonitis often improves within a few weeks to several months, depending on severity. Rest, activity modification, and following a treatment plan are key to recovery.
Swelling from Diabetic Foot Care Complications
In people with diabetes, swelling in the feet can indicate circulation problems, nerve damage, infection, or other complications. Because diabetes can reduce sensation in the feet, swelling may go unnoticed and worsen without prompt care, making early evaluation especially important.
In addition to swelling, common symptoms include:
- Redness
- Warmth
- Skin changes
- Sores or wounds that heal slowly
In some cases, there may be little to no pain, which is why regular foot checks are critical for individuals with diabetes.
Recovery depends on the underlying cause of the swelling and how quickly it is treated. Mild issues may improve within weeks with proper foot care, blood sugar management, and medical treatment, while more serious complications, such as infections or ulcers, can require ongoing care and longer recovery periods.
Prompt treatment is essential to prevent further complications and support long-term foot health. As Physicians Footcare podiatrist Dr. Kevin Uren says, “Diabetics out there: Take care of your feet, and they will take care of you.”
Understanding Your Symptoms and Next Steps
Swollen feet can range from a mild inconvenience to a sign of a serious medical condition. Understanding what causes swollen feet, monitoring changes, and recognizing when swollen feet may be dangerous can help you make informed decisions about your health. Paying attention to your body, scheduling annual foot doctor visits, and seeking medical guidance when something doesn’t feel right are the best ways to protect your foot health and address concerns before they become more serious.
If swelling persists, worsens, or is accompanied by other concerning symptoms, it’s important to seek professional care. At Physicians Footcare, our experienced podiatrists specialize in diagnosing and treating the underlying causes of foot and ankle swelling. With convenient locations across South Carolina and advanced diagnostic technology available in-office, our team can quickly evaluate your symptoms and recommend the most effective treatment plan..
If you’re unsure when to worry about swollen feet, connecting with one of our doctors can help ensure you receive the right care at the right time. Reach out to Physicians Footcare today to protect your foot health and overall well-being.
Physicians Footcare Welcomes Dr. Farah Lakhram

Dr. Lakhram is certified by the American Board of Podiatric Medicine and licensed in several states. She is an experienced doctor with a breadth of experience servicing the footcare needs of pediatric to geriatric patients.
“We are excited to welcome Dr. Lakhram to our practice,” said Dr. Ray, CEO, Physicians Footcare. “Her diverse background, including clinical, hospital, and research experience, will provide immense benefit to our patients. We look forward to her contributions in providing comprehensive foot and ankle care.”
“I am excited to join Physicians Footcare and contribute to the established legacy of patient-first care. I look forward to using my knowledge and expertise about foot health to assist patients in performing their daily activities with ease,” says Lakhram.
To schedule an appointment with Dr. Lakhram, contact our Florence or Orangeburg Office toll-free at 1-833-PFC-FOOT. To learn more about Physicians Footcare and the array of healthcare services we provide, visit www.physiciansfootcare.com.
About Physicians Footcare
Physicians Footcare is one of the largest podiatric practices in the southeast and the nation. It is the Southeast’s premier podiatry practice, independently and privately owned. Since opening our first location in 2006, we have grown to locations in South Carolina, Georgia, and New York. Our mission is simple: to be the Best Medical Practice.
Physicians Footcare Welcomes Dr. King-Adekunle
 Aiken, SC- Physicians Footcare, the Southeast’s premier podiatric practice, is pleased to announce that Dr. Dorinda King-Adekunle will be joining our team. She will begin treating patients in our Aiken office on February 2, 2026.
Aiken, SC- Physicians Footcare, the Southeast’s premier podiatric practice, is pleased to announce that Dr. Dorinda King-Adekunle will be joining our team. She will begin treating patients in our Aiken office on February 2, 2026.
Dr. King received an MBA in health and medical services from Widener University and a doctorate of Podiatric Medicine from Temple University. She is board-certified in primary podiatry medicine and a member of the American Board of Multiple Specialties in Podiatry.
Dr. Ray, CEO, Physicians Footcare stated, “We are happy to welcome Dr. King to Physicians Footcare. Her diverse healthcare background and recognition of foot health as whole health will be invaluable to our patients.”
“I am elated to join the Physicians Footcare Team and to help serve the podiatric needs of the Aiken community,” says King. “My patient-centered approach to care and over two decades of experience in the medical field will help me keep this community in motion.”
To schedule an appointment with Dr. King, contact our Aiken Office toll-free at 1-833-PFC-FOOT. To learn more about Physicians Footcare and the array of healthcare services we provide, visit www.physiciansfootcare.com.
About Physicians Footcare
Physicians Footcare is one of the largest podiatric practices in the southeast and the nation. It is the Southeast’s premier podiatry practice, independently and privately owned. Since opening our first location in 2006, we have grown to locations in South Carolina, Georgia, and New York. Our mission is to be the provider of choice for quality podiatric surgical and medical services and recognized for extraordinary patient care experiences for acute and chronically injured patients and their families.
Why Do I Feel Unstable on My Feet? Foot Instability & Balance
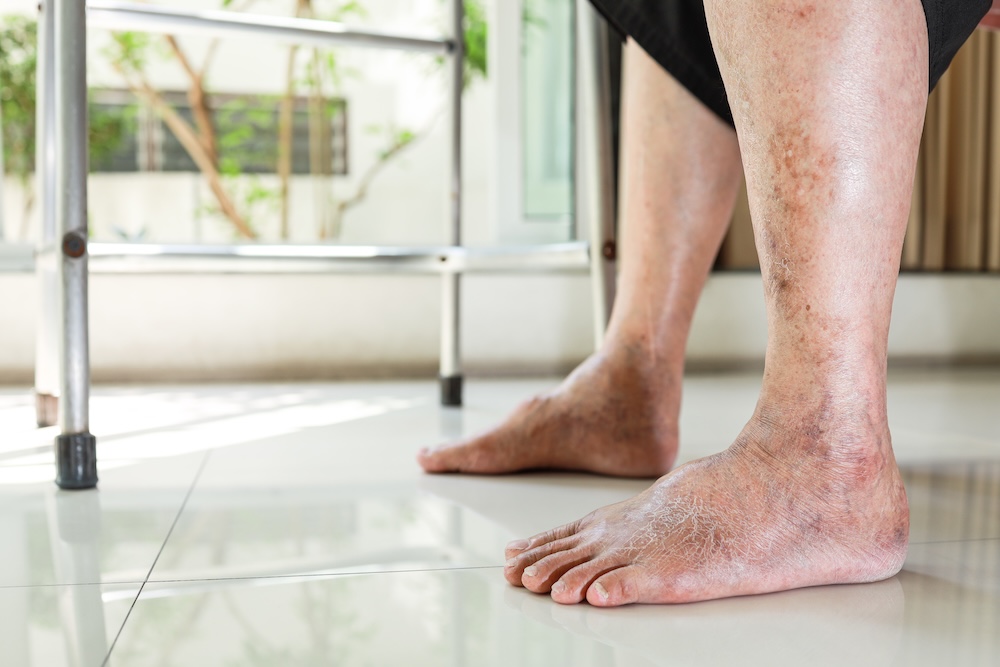 Balance plays a significant role in daily movement and independence, and foot instability is a common, yet often overlooked, reason people begin feeling unstable on their feet. From moving safely throughout your home to running errands or enjoying time with family, feeling steady on your feet is essential for both your confidence and safety.
Balance plays a significant role in daily movement and independence, and foot instability is a common, yet often overlooked, reason people begin feeling unstable on their feet. From moving safely throughout your home to running errands or enjoying time with family, feeling steady on your feet is essential for both your confidence and safety.
Falls are especially concerning for older adults. They are one of the most preventable health risks, yet they can still have serious consequences. A fall can lead to broken bones, permanent loss of mobility, reduced independence, and prolonged recovery periods. For many families, it’s not just physically challenging for the patient, but also emotionally difficult to watch a loved one struggle to recover after an injury.
Understanding the role foot instability plays in balance is a key step towards prevention, early treatment, and long-term mobility.
Why Is Foot Stability Critical for Balance and Fall Prevention?
Balance and stability are essential for maintaining independence. Good balance helps your body stay upright and respond quickly to changes in your environment, such as uneven ground, obstacles, or sudden movements.
Benefits of good balance include:
- Stronger stabilizing muscles
- Faster reaction times
- Improved coordination
- Better posture and joint alignment
- Greater confidence and independence
Body balance, also known as equilibrium, is maintained through sensory input that tells the brain where the body is in space. One of the most important inputs is proprioception. This is the sensors in your muscles and joints that send constant data to the brain for instant postural adjustments.
This system allows your body to maintain its center of gravity over its base of support during standing, walking, and changing positions. When this system functions well, it allows smooth, confident movements and reduces hesitation, missteps, and instability while moving. It also supports quicker balance corrections when navigating uneven surfaces or sudden changes in direction. When foot instability interferes with this neurological process, balance becomes much harder to maintain.
Why Do I Feel Unstable on My Feet When Walking or Standing?
Foot instability can disrupt balance by reducing the quality of information sent from the feet to the brain. The feet are constantly collecting sensory data about pressure, surface texture, and body position. When this feedback is delayed, weakened, or distorted, the brain receives incomplete information. This makes it harder for the body to respond quickly to changes in position or uneven surfaces, increasing the risk of losing balance and falling.
The feet act as the foundation for the entire body, directly influencing joint alignment through the ankles, knees, hips, and spine. Poor foot stability can lead to misalignment and inefficient movement patterns, increasing stress on joints and contributing to feeling unstable on feet, especially during daily activities.
Key Foot Components That Affect Foot Instability and Balance
- Enhanced Proprioception: The feet contain thousands of nerve endings that send essential signals to the brain about pressure, position, and movement. Strengthening the feet improves the sensitivity of these nerves, allowing for better grounding and control during movement.
- Toe strength: Toes act as an anchor and provide stability during standing and walking. The big toe plays a particularly important role, accounting for up to 40% of overall foot stability. Weak toe strength is a common cause of feeling unstable on your feet.
- Ankle stability: The ankle serves as the foundational joint for shock absorption, weight support, and proprioceptive feedback. Strong and stable ankles help control body position on uneven surfaces. Limited ankle strength and mobility can make foot instability worse and increase fall risk.
How Declining Foot Strength Leads to Feeling Unstable on Your Feet
As foot strength and sensory feedback decline, balance becomes significantly less reliable. Reduced input from the feet can delay reaction times, weaken postural control, increase anxiety, making it harder to recover quickly from a loss of balance.
Over time, everyday movements like turning, stepping off a curb, walking on uneven flooring, or standing up from a chair may begin to feel uncertain. Muscle fatigue, stiffness, or poor alignment can further amplify the problem, causing individuals to subconsciously shorten their stride or avoid certain movements altogether.
These compensations can further worsen foot instability and increase the risk of trips, missteps, and falls during daily activities.
How to Improve Balance and Stop Feeling Unstable on Your Feet
Improving balance often starts with addressing daily habits and foot health:
- Vision checks to ensure good eyesight and confidence while moving
- Safe footwear with strong, balanced soles, a proper fit, and secure laces
- Hydration, which supports circulation, muscle function, and nervous system performance
- Regular foot strengthening and mobility exercises
These steps can be a critical factor in reducing your foot instability and improving overall balance.
Exercises to Make Your Feet Stronger
Improving balance begins at the source - the feet. Simple, regular exercises can help reduce foot instability and restore confidence.
- Towel scrunches: Sit with flat feet on a towel and scrunch it toward you using your toes. Repeat 10-20 times.
- Toe splay: Sit with heels on the floor and toes pointed upward. Spread toes wide and hold for 5 seconds. Repeat 10 times.
- Marble pick-ups: Use your toes to pick up small objects (like marbles) and place them into a bowl. Repeat 10-20 times.
- Ankle circles: Lift one leg and rotate the ankle 10 times clockwise and 10 times counterclockwise.
- Calf raises: Hold onto a chair or wall, rise onto your tiptoes for 5 seconds, then lower. Repeat 10 times.
Exercises that focus on toe strength, arch support, and ankle stability can lead to meaningful improvements in balance and reduce the sensation of feeling unstable on the feet.
As Physicians Footcare CPed Natalie McCoy says, “Our furry friends, cats/dogs, have an instinct to stretch every time they get up, so why don't we? Stretching is a preventative action we should all be doing daily, just like brushing our teeth. Stretching daily can help prevent overuse injuries and has great health benefits. Remember: motion is lotion.”
How A Podiatrist Can Help Improve Foot Instability
If you continue to feel unstable on your feet, it may be time to see a podiatrist. A podiatrist can evaluate underlying conditions that may affect your balance, such as:
- Peripheral neuropathy
- Arthritis
- Flat feet or structural imbalances
- Tendon or ligament weakness
At Physicians Footcare, we take a comprehensive approach to balance concerns. Your personalized treatment plan may include targeted exercises, custom orthotics, footwear recommendations, pain management strategies, physical therapy, and ongoing care to support safer movement and long-term stability.
Custom Orthotics for Foot Instability and Balance Support
One of the most common ways podiatrists improve foot stability and ankle alignment is through custom orthotics and shoe inserts. By redistributing pressure and providing targeted support, orthotics help create a more stable base and improve balance during daily activities like standing and walking.
Our certified pedorthist team at Physicians Footcare specializes in creating custom inserts tailored to your unique foot structure, gait, and stability needs. These custom devices can help improve alignment, enhance sensory feedback from the feet, and reduce strain on the ankles, knees, and hips.
Stronger Feet Lead to Safer Movement
Balance starts from the ground up. Addressing foot instability early can help prevent falls, maintain independence, and support safer movement at every stage of life.
Foot instability doesn’t happen overnight, and it doesn’t have to be faced alone. If you’re asking yourself, “Why do I feel unstable on my feet?” Physicians Footcare can help you find answers, solutions, and move with confidence again.
Welcome Dr. Joon Kim to Physicians Footcare
Savann ah, GA- Physicians Footcare, the Southeast’s premier podiatric practice, is pleased to announce that Dr. Joon Kim will be joining our team. He will begin treating patients in our Aiken office on January 19, 2026.
ah, GA- Physicians Footcare, the Southeast’s premier podiatric practice, is pleased to announce that Dr. Joon Kim will be joining our team. He will begin treating patients in our Aiken office on January 19, 2026.
Dr. Kim is a board-certified member of the American Board of Podiatric Medicine and is board-qualified with the American Board of Foot and Ankle Surgery. He and his family moved from South Korea to the United States when he was eight years old and proudly considers Gainesville, FL, home. Dr. Kim attended the University of Florida for his undergraduate studies and is an honors graduate of Kent State University College of Podiatric Medicine. Following graduation, he completed a podiatric medicine and foot and ankle surgery residency at Mt. Sinai Medical Center in Miami, Fl.
“I am honored to join Physicians Footcare and look forward to addressing the footcare needs of the Aiken community”, says Kim. “In my position, I will continue emphasizing a personalized approach to foot health using the least invasive and most advanced techniques for the maximum results.”
Dr. Ray, CEO, Physicians Footcare, stated, “We are excited about the addition of Dr. Kim to our team. His diverse background and extensive knowledge about the breadth of footcare, including diabetic foot care, wound care, sports medicine, regenerative medicine, and foot and ankle surgery, will be a welcome addition to the Augusta-Aiken Region.”
To schedule an appointment with Dr. Kim, contact our Aiken Office toll-free at 1-833-PFC-FOOT. To learn more about Physicians Footcare and the array of healthcare services we provide, visit www.physiciansfootcare.com.
About Physicians Footcare
Physicians Footcare is one of the largest podiatric practices in the southeast and the nation. It is the Southeast’s premier podiatry practice, independently and privately owned. Since opening our first location in 2006, we have grown to locations in South Carolina, Georgia, and New York. Our mission is to be the provider of choice for quality podiatric surgical and medical services and be recognized for extraordinary patient care experiences for acute and chronically injured patients and their families.
Foot Safety at Work: How to Protect Your Feet on the Job

Workplace environments place constant physical demands on the body. In particular, your feet absorb impact, maintain balance, and support movement during every task. Whether you’re standing for long hours, navigating uneven surfaces, or working around heavy equipment, your foot health has a direct impact on comfort, foot safety, and job performance. Addressing foot protection early helps set the stage for safer workplaces and reduces the risk of injuries that can affect both your short-term productivity and long-term mobility.
The Foundation of Workplace Safety Starts at Your Feet
Workplace foot protection is fundamental to overall workplace safety, serving as the first line of defense against many job-related hazards. Your feet provide the structural base for balance, stability, and movement. This makes them especially vulnerable to injury in physically demanding work environments — and it means that foot safety at work is critical to your overall comfort and mobility.
When you experience fatigue, instability, or foot pain at work, your ability to perform tasks safely and efficiently is compromised. Poor footwear can contribute not only to foot and ankle injuries but also to knee, hip, and lower back strain due to altered gait and posture. Over time, these issues may lead to increased absenteeism, reduced job performance, and a higher risk of secondary injuries.
Why What You Wear on Your Feet Matters at Work
The type of footwear you wear on the job plays a critical role in both injury prevention and overall physical performance. Inadequate footwear—such as shoes that lack proper support, traction, or protective features—can significantly increase the risk of foot injuries in the workplace. Over time, poorly designed or ill-fitting shoes contribute to excessive pressure, instability, and repetitive stress on the feet.
Footwear that does not provide adequate protection leaves workers more vulnerable to acute trauma, including impact injuries, puncture wounds, and slip-related accidents. Repetitive strain and insufficient support can also contribute to ongoing foot stress, particularly in roles that require prolonged standing or walking. These issues may gradually affect movement patterns, stability, and endurance throughout the workday.
Proper protective footwear helps reduce these risks by supporting natural alignment and absorbing impact during daily work activities. Shoes designed with appropriate cushioning, arch support, slip-resistant soles, and protective features improve posture and balance, allowing workers to move with greater confidence and control. By enhancing stability and reducing fall risk, the right footwear supports foot safety at work and long-term musculoskeletal health.
As Physicians Footcare podiatrist Dr. Renee Hutto-Altman says, “Just because your friend or neighbor likes a certain shoe does not mean it is a good shoe for your foot!” Make sure you try on your work shoes before purchasing, and make sure they feel comfortable and supportive for you.
Common Workplace Foot Injuries Podiatrists See
Despite advances in workplace safety and foot protection, foot injuries remain a common reason workers seek podiatric care. Many of these injuries are directly related to job-specific hazards, repetitive stress, or prolonged time spent on hard surfaces. Understanding the most frequent workplace foot injuries can help workers and employers recognize risks early and improve foot safety on the job.
Acute Workplace Foot Injuries
These injuries often occur suddenly and are typically linked to environmental hazards or inadequate protection:
- Crushing injuries and fractures caused by dropped tools, equipment, or heavy materials
- Puncture wounds and lacerations from sharp debris, nails, or uneven surfaces
- Slip and fall injuries related to poor traction, wet floors, or unstable footing
Overuse and Repetitive Stress Injuries
Jobs that require prolonged standing, walking, or repetitive movement can lead to cumulative stress on the feet over time, including:
- Plantar fasciitis resulting from repeated strain on the heel and arch
- Tendinitis caused by overuse of the muscles and tendons that support foot and ankle movement
- Nerve pain in the feet from standing, often described as burning, tingling, or numbness
- Workplace foot fatigue, which can reduce stability, focus, and overall job performance
Early identification and proper treatment of these injuries are essential for preventing chronic pain and long-term mobility issues. Appropriate footwear, workplace modifications, and timely podiatric evaluation play a key role in keeping workers safe, comfortable, and productive on the job.
Types of Safety Footwear for Different Jobs
When footwear inadequately supports or protects the feet, the impact is often seen over time. Daily exposure to workplace hazards, combined with repetitive movement and prolonged standing or walking, places significant stress on the feet. Because many workplace foot injuries stem from job-specific hazards, selecting the right type of safety footwear is essential for foot protection and long-term foot health.
Protective Toe Footwear
- Steel-toe boots offer maximum protection against heavy falling or rolling objects and are commonly used in construction, manufacturing, and industrial settings.
- Composite toe shoes provide similar protection while being lighter in weight and non-metallic, making them a popular option for workers who require comfort, temperature resistance, or metal-free environments.
Slip-Resistant Work Shoes
- Designed for healthcare, hospitality, and food service environments where wet or slick floors are common.
- Help reduce slip-and-fall injuries by improving traction and stability during long shifts.
- Often feature lightweight designs to support extended periods of standing and walking.
Puncture-Resistant Footwear
- Equipped with reinforced soles to protect against nails, sharp tools, and debris
- Recommended for construction sites, warehouses, and outdoor job settings
- Helps prevent serious injuries caused by penetrating objects
Electrical Hazard Footwear
- Designed to reduce the risk of electrical shock in high-risk environments
- Used by electricians, utility workers, and those working around live electrical equipment
- Must meet specific safety standards to provide appropriate protection
The Importance of Proper Fit and Support
Regardless of job type, proper fit and supportive features are critical to injury prevention. Footwear that is too tight, too loose, or lacks adequate structure can increase fatigue and strain. Features such as arch support, cushioning, and shock absorption help distribute pressure evenly and support natural movement, reinforcing both foot safety and comfort throughout the workday.
Choosing the appropriate safety footwear for the job not only protects against immediate hazards but also supports comfort, stability, and long-term musculoskeletal health.
How to Choose the Right Safety Footwear for Your Job
Choosing the right footwear requires more than selecting a safety label. Effective foot protection at work depends on matching footwear features to job-specific hazards while also addressing comfort, fit, and long-term foot health.
Understanding OSHA (Occupational Safety and Health Administration) foot protection requirements is essential, but meeting minimum standards does not always prevent discomfort or fatigue. Many workers find that “one-size-fits-all” safety shoes contribute to ongoing discomfort and wonder how to stop foot pain at work. Poor fit, limited support, and insufficient cushioning can increase strain even when footwear meets safety guidelines.
In cases where standard safety footwear falls short, custom orthotics or medical-grade inserts may be recommended. These devices are designed to improve support, distribute pressure more evenly, and reduce strain during prolonged standing or walking. At Physicians Footcare, custom orthotics are available, and our on-site pedorthists specialize in evaluating footwear fit and designing orthotic solutions tailored to each individual’s job demands and foot structure. This personalized approach helps workers achieve both protection and comfort, supporting safer, more sustainable performance at work.
Foot Pain on the Job: When Discomfort Signals a Problem
Even with appropriate safety footwear, foot pain should never be dismissed as a normal part of the workday. Discomfort is often an early warning sign that the feet are under excessive stress or that foot protection needs are not being met. Recognizing these symptoms early allows workers to address problems before they interfere with safety, performance, or long-term mobility. Workers should pay close attention to symptoms such as:
- Persistent heel or arch pain that does not improve with rest
- Burning or tingling sensations, particularly after long periods of standing or walking
- Swelling, numbness, or feelings of instability during movement
Ignoring these warning signs can allow minor issues to progress into chronic injuries that require more extensive treatment and recovery time. Ongoing foot pain may alter posture and movement patterns, increasing strain on the ankles, knees, hips, and lower back. Over time, this can lead to reduced productivity, increased risk of falls, and time away from work.
Seeking a podiatric evaluation is recommended when foot pain is persistent, worsening, or interfering with daily job duties. Early assessment allows for timely intervention, footwear adjustments, or supportive therapies that can help workers stay comfortable, mobile, and safe on the job.
Supporting Workplace Safety from the Ground Up
Proper foot protection at work does more than safeguard the feet; it supports mobility, longevity, and overall quality of life. When workers wear footwear designed to protect and support their feet, they are better equipped to move safely, maintain balance, and reduce strain throughout the workday. Over time, these benefits extend beyond injury prevention, helping preserve long-term musculoskeletal health and on-the-job performance.
Prioritizing podiatrist-approved footwear is an important step for both workers and employers committed to workplace safety. Selecting shoes that match job demands, fit properly, and provide appropriate support can significantly reduce the risk of foot injuries while promoting comfort and stability. Professional guidance ensures that foot protection addresses both safety requirements and individual foot health needs.
At Physicians Footcare, our team is dedicated to helping workers prevent foot injuries and maintain healthy, pain-free movement. Whether you are seeking guidance on workplace footwear, custom orthotics, or strategies for how to stop foot pain at work, our podiatric physicians and specialists are here to help. Contact Physicians Footcare today to take a proactive step toward protecting your feet—and your future—from the ground up.
