Connect with us:
Blog
Items filtered by date: December 2019
Choosing Running Shoes for New Runners | Demond Thompson, C.Ped
New year, New resolutions…. For those of us that has chosen running as one of those resolutions, we are pretty excited to get out and put in some miles, but before you start pounding the pavement and chasing those miles, lets make sure you have the proper running shoes. Running is a simple beauty, and the benefits of a well fitted running shoe can make all the difference in the world.
When trying on running shoes they will often feel comfortable while you’re standing in the shoe store, but the true test comes after several miles into your run. Understanding your running style and foot type will benefit you in choosing the right running shoes. When it comes to running shoes, how they fit is one of the most important factors to consider. An ill-fitting running shoe will not only make your running experience painful, it may also cause you to change your stride, leading to potential injury. Your feet tend to spread as you run. They also tend to swell a bit throughout the day, so trying on your shoes in the afternoon or evening may provide a more accurate fit. To accommodate foot spread, there should be roughly one thumb width between the end of your longest toe and the end of the shoe. Your shoes should wrap comfortable around your feet, they should not pinch or feel sloppy, and your feet should be centered on the platform of the shoes. Some shoes may better accommodate a narrow or wide foot, additionally, some shoe models are available in either wider or narrower size options. Standard shoe widths are Wide for men and Medium for women.
When choosing a running shoe, consider your style of running: trail running, cross training or road running.
- Road running shoes are designed for pavement, they’re usually light and made to cushion and stabilize your feet on hard surfaces.
- Trail running shoes are designed with aggressive treads that provides solid traction, stability, and protection while running off road on uneven terrain, such as rocks, mud, roots or other obstacles.
- Cross trainers are designed more so for gym type workouts. These shoes are designed to give you more contact with the ground more so then the previous mentioned shoes, due to their thicker platform.
How do you run? Knowing how you run is very important when choosing the right running shoes. If you have an old pair of running shoes check the wear pattern to help you determine your running mechanics.
- Neutral Foot: The wear pattern you will see in for this foot type is a wear pattern centralized to the ball of the forefoot and a small portion of the out side heel (The right side of the heel if you’re looking at the right shoe from the back, and the left side of the heel if you’re looking the left shoe from the back). This pattern shows the foot’s natural heel strike, to mid stance to toe off (your gait). The neutral foot type helps absorb impact, by relieving pressure on the knees, hips and lower back. It is the normal trait of biomechanically efficient runners.
- Overpronation (Flattening of the arch) The wear pattern you will see in this foot type is a wear pattern along the inside edge of your shoes. The wear pattern will be medially located to the forefoot and rear foot (this will be the right side of the left shoe under the big toe and the heel, and the left side of the forefoot and heel of the right shoe if you’re looking at the shoes from the back). Overpronation is one of the most common foot types that affects runners, this foot type can leave runners risk of knee pain/ injury, heel pain, Achilles tendon pain/ injury ect. This foot type need stability or motion control shoes.
- Supination (High arch): The wear pattern you will see in this foot type is a wear pattern along the outside edge of your shoes. Very few runners supinate, but those who do will benefit from a shoe with plenty of cushioning and flexibility.
Running can be rewarding, fun, and relaxing, but it also can cause a lot of harm if you’re not in properly fitted shoes. For more information, contact us for a free gait and foot evaluation today.
Your New Year's Diet May Affect Your Feet | Abbasova, DPM
It is the beginning of a new year and gyms are once again packed with enthusiasm. Space is becoming limited in and yoga and barre studios. The sales of books preaching paleo, vegan and ketogenic eating diets spike and you find yourself trying to figure out which direction to take your fitness and health goals.
While every nutrition program may come with its benefits, most people rarely take a moment to evaluate the effects that diet may have on our legs and feet. A Western diet, with which most of us are familiar, is rich in carbohydrates such as bread, rice, pasta and potatoes. In order to maintain a steady blood glucose level for healthy function, the pancreas works restlessly to pump out insulin, which is critical in shuttling the glucose out of the blood and either to our muscles and brain to be utilized or to be converted into energy reserves as glycogen or fat. A high carbohydrate diet is essentially a high glucose diet at the metabolic level and has your body—more specifically your pancreas—working very hard to keep the balance. The pancreas, like any other organ, is at risk to wear out if overworked. Another serious consequence of constantly elevated glucose and insulin levels is resistance to insulin, which occurs as the insulin sensitivity in the muscles decreases. We see a steady rise in diabetes as a direct consequence of the Western diet with devastating effects on the neurovascular system leading to thinning brittle skin, peripheral vascular disease and neuropathy.
Choosing a diet high in protein and increasing intake of meat and fish may help with controlling insulin spikes, blood glucose and appetite. However, the high protein diet may not be best for everyone due to the increase in uric acid level that would be added to the diet. Most animal derived protein has high levels of uric acid and people with decreased ability to excrete the acid or people who are natural overproducers of uric acid may develop a painful condition of Gouty Arthritis, better known as “Gout”. The common symptom of a Gout attack is a red, hot and swollen joint. The condition is commonly isolated to one joint at a time as the uric acid condenses into crystals, which leads to pain and joint erosion. In the foot, it is commonly the first metatarsophalangeal joint proximal to the great toe.
Some people may consider adopting a vegan or a vegetarian diet for ethical, environmental or the health benefits. It is important to keep in mind that Vitamins B6, B12 and folic acid are essential for healthy functioning blood cell and myelination, the covering of nerve cells. A strict vegetarian diet would promote a B12 deficiency as animal based foods such as red meat, dairy products, fish, poultry and eggs are the only recognized source of dietary B12. Without proper oral or injectable supplementation, eliminating animal derived food products may put one at risk for anemia and serious nerve damage leading to neuropathy. One of the first symptoms of neuropathy is the tingling and numb sensation of the feet.
Most Americans cite lack of time as the reason to have neglected making healthier choices. The savvy entrepreneurs noticed a need and there are now many options for delivery companies that will help you with your dinner plans. Walking down the aisle of your local grocery store frozen foods section, you notice that there is no lack of options for convenience foods. The controversial topic of preservatives aside, we need to be cautious of the sodium in conveniently packaged foods. While prepackaged meals advertised as healthy can help us with controlling the calorie intake, the increase in sodium may contribute to swelling and aches of the legs and feet that some people feel at the end of a long day.
It is possible that the change in your diet is the reason for an inflamed joint, swelling of the legs and feet or the tingling sensation of your toes, but taking your health to online research is never enough. It is essential that you speak with your medical and foot care provider about these symptoms. Your provider will help with narrowing down the differential diagnoses for the symptoms of the neuropathy and you may need follow-up testing or imaging for appropriate treatment. Of course, it is recommended to consult your provider before making significant changes to your diet and/or level of physical activity.
What To Do If You Have Flat Feet
Flatfoot is a foot condition in which the arch of the foot has either partially or totally dropped or has never developed. While it is common in babies and small children, it can become a problem for them in adulthood if the arch never forms. For adults, the development of flat feet can be brought upon by injury, as a result of pregnancy due to increased elasticity, or obesity. Those who have health concerns such as rheumatoid arthritis or diabetes may also be at greater risk for developing the condition.
If you suspect that you have flat feet, it is best to consult your podiatrist. Your foot doctor will examine the suspected foot and observe how it looks while you sit and stand. He or she may take an X-ray to determine how serious the condition is. Some common signs of flatfoot include toe drift, in which the toes and front part of the foot point outward, a short Achilles tendon, and a heel that tilts outwardly while the ankle tilts inward.
Once flatfoot has been diagnosed, your podiatrist may suggest one of several treatment options. Flat feet can be rigid, in which the feet appear to have no arch even when the person is not standing; or flexible, in which the person appears to have an arch while not standing, but once standing the arch disappears. Those with flexible flatfoot may be told to reduce any activities that cause pain and to avoid extended periods of walking or standing. Another suggestion may be weight loss, as excessive weight may be placing pressure on the arches
In few cases, if the condition is severe and all other methods have been exhausted surgery may be required. This is normally avoided, however, due to a lengthy recovery time and high cost.
Pick Up More Than Weights at the Gym? Let’s Talk Foot Fungus
In the medical field we deal with a variety of problems. Often in TV shows the focus is on life or death situations, big accidents, and well allot of drama. However most of the time the focus is on eliminating pain or an uncomfortable feeling so that our patients can live fulfilling pain free lives, doing the activities they love. Foot fungus or tinea pedis can present in a variety of ways, from extremely painful blisters a rash or even as painless flaky skin. No matter the presentation we often find that this disease impacts our patients in a negative manner. Some times the pain makes work impossible, or some times the appearance makes patients embarrassed to do something as simple as taking a walk on the beach without shoes. Regardless of which group you fall into there is not only something that can be done but should be done. Studies have shown that the presence of foot fungus regardless of the severity has been linked to other conditions such as: nail infections, leg cellulitis, and diabetic foot syndrome. This article will tell you not only what to look for but what to ask your doctor about.
Foot fungus is now the most common type of identified fungal infection. Names for it include: tinea pedis, ringworm, and dermatophyte infection. Regardless of which name you hear they mean the same thing. Foot fungus is contagious and often is spread to a susceptible host. This can occur through a communal shower, sharing socks or shoes, or any shared surface that you do not have shoes on. However not everyone who comes into contact with fungus will get the infection. There is research indicating that the host must be susceptible to the infection, based on a variety of genetic factors. However being tested for these genetic factors is not feasible at this time, and for that reason it is better to avoid any areas where they may come into contact or at least mitigate their risk. Mitigating risk involves wearing socks and shoes whenever possible. When not possible wear sandals and avoid the bare foot from making contact with any surfaces. There are 3 main types of foot fungus that you should be aware of. 1st is interdigital tinea pedis. This is marked by itching between the toes, or of the entire foot. Also there is often maceration or increased moisture of the skin between the toes. If this type of tinea pedis is severe enough there is often noted ulcers, and skin sloughing, accompanied by a foul odor. The second type of tinea pedis that you should be aware of is dry tinea pedis. This infection often starts on the botom of the feet and may have some redness and flaky skin. However as the infection develops the body responds by creating more keratin, which may thicken the skin and even lead to cracks in the skin. Finally the 3rd type of foot fungus is vesicular tinea pedis. This fungal infection starts as a superficial flaking of the skin. As it progresses deeper there is noted infiltration of the skin leading to small raised clear bumps or blisters. It is important to note that these vesicles may be painful or pain free. This can also lead to a bacterial infection. If they do become infected with a bacteria in addition to the fungus there will often be an accompanying smell or drainage. This concludes the 3 most common types of tinea pedis that are enountered though there are a variety of other infections that can occur.
As seen there is a large variety of foot fungus with different presentation. It is also known that they can lead to much more severe problems than a bad appearance. For this reason it is important that when you see your podiatrist ask them if your dry feet might be infected. Tell them if you ever notice any redness, flaking, or itching of the feet. Tell them abut what shoes you wear, how long you are in them and if you notice that your feet are wet at the end of the day. Try to inform them if you notice an odor. Ask them if there office performs fungal cultures. This is particularly helpful in the earlier stages of fungal infections as noted above they may start off as very mild peeling of the skin. This will help determine if what you have going on is a reaction of your skin to an irritant, a fungal infection, or possibly just dry skin or xerosis. Finally ask them about ways to prevent infection as not all talking points were covered in this article. Patient treatment is often a conversation about what is going on and ways that not only we as physicians can treat the problem, but ways the patients can focus on the problem on a daily basis.
What Causes Plantar Fasciitis?
The plantar fascia is a connective tissue in the heel that stretches across the bottom length of your foot. Plantar fasciitis occurs when the connective tissue becomes inflamed, causing heel pain and discomfort during physical activity. Although the condition is completely treatable, traditional methods can take up to a year to start becoming effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding the condition is important for managing and treating it. One of the most common causes of plantar fasciitis is excessive running, especially with improper fitting or non-supportive shoes. Too much exercise can lead to the plantar fascia being overworked and overstretched, which can cause tears in the tissue. Along with improper fitting shoes, pronation, the rolling of the feet inward, is a common cause of plantar fasciitis. If not treated properly, the plantar fascia becomes overstretched and starts to tear, causing inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options. For less severe cases, conservative home remedies include taking anti-inflammatory drugs to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching and exercising your feet to re-strengthen the tissue, and using orthotic devices are all ways to help manage your plantar fasciitis.
For more severe cases, shockwave therapy has become a common solution for plantar fasciitis. Shockwave therapy can effectively break up the tissue on the bottom of your foot which facilitates healing and regeneration. This fights the chronic pain caused by plantar fasciitis. Even if this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be done to permanently correct the issue and stop the inflammation and pain in your heels.
No matter what the case may be, consulting your podiatrist is the first and best step to recovery. Even the slightest amount of heel pain could be the first stage of plantar fasciitis. Untreated symptoms can lead to the tearing and overstretching of tissue. Because the tearing of tissue can be compounded if it remains ignored, it can evolve into a severe case. The solution is early detection and early treatment. Talk to your podiatrist about the possibilities of plantar fasciitis if you’re experiencing heel pain.
Grand Opening Event
Join Physicians Footcare and Foot Solutions for our Grand Opening celebration. We will have raffles, giveaways, special discounts and offers!! Get a free foot analysis. Tour our new facilities and meet our team of doctors and staff.

Every Day Foot Care
Our feet are important in our everyday lives. The problem is that we tend to neglect them. When this becomes a habit, it can cause significant trouble. Ignoring foot problems can mean pain, limited mobility, and expensive doctor's visits. On the other hand, if feet are cared for and looked after regularly, they will perform without pain or complication.
Routine hygiene is the most basic way to care for the feet. Wash and dry them thoroughly daily. Remember to get between the toes and keep the toenails trimmed and short. If the feet feel dry or there are signs of dryness or cracking, use a moisturizer designed for the feet.
When using moisturizer on the feet, try to avoid applying between the toes. If cream or lotion sits too long, they can cause fungal and bacterial growth. When moisturizer is used between the toes, it can also cause the skin to soften too much.
Shoes are also an important aspect of foot care. When one is picking out shoes, make sure they are the correct size. Shoes need to be snug, but not too tight. On the other hand, if shoes are too loose they can cause foot problems as well. It is highly recommended that shopping for new shoes be done later in the day. The reason for this is that the feet will have settled and swelled to their full size by then. To keep your feet at their most healthy, avoid wearing high heels or flip flops too often. Instead, choose shoes that are good for your feet. Good shoes pad the soles of your feet and support the arches and ankles.
Socks should also be worn daily with closed-toe shoes. They may feel hot during the summer months, but they absorb sweat and moisture off the feet. Without socks, the build-up of sweat in a closed-toe shoe can cause fungal problems and athlete's foot.
The best thing to remember in every day foot care is that shoes do make a difference. If you spend a lot of time on your feet, make sure that your shoes show no signs of wear. Shoes should offer ample support for the arches and the overall foot. Additionally, try to make foot cleaning and maintenance a daily habit. If you keep these things in mind, your feet will stay healthy and safe.
Do You Have Nail Fungus? That’s A Shame! | Renee Hutto-Altman, DPM
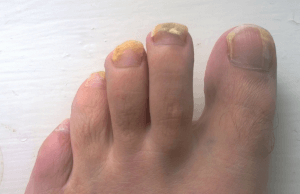
DO YOU HAVE NAIL FUNGUS? THAT’S A SHAME!
If you have nail fungus, you are ready to hide your toes! Physicians Footcare wants you to show them to the world after we have helped to treat this problem.
What are some signs of nail fungus? Lifting of the nail from the nail bed, changes in color, brittle nails, extra skin under the nails.
Can it become serious? Fungus can spread from nail to nail and is contagious to others in yourhousehold. Other complications include loss of the nail, bacterial infection, and recurrence after treatment.
Is it preventable? YES! Make sure you don’t go barefoot in public places (gyms, hotels, pools). Don’t share shoes or purchase used shoes. Be very cautious of nail salons and look at the feet of your family members to make sure they don’t have a problem.
Is it treatable? Yes, it is! At Physicians Footcare, we will confirm the diagnosis, and recommend treatment based on your medical history. Treatments include creams, nail lacquers, laser, and oral treatment. Your physician will also instruct you regarding the best shoe and sock hygiene.
Don’t delay. Get ready for summer and call a Physicians Footcare office near you to schedule your consultation. We are ready to help! www.physiciansfootcare.com
Let’s Talk About Stress . . . Fractures | Jamelah Lemon, DPM

The temperatures are dropping as we enter into the cooler seasons of fall and winter which usually means we put away our sandals and bring out our boots. In the cooler months, some hospitals report up a 500% increase in ER visits usually due to slips and falls. Stress fractures, a hairline crack in the bone of the foot, are one of the more common winter-related injuries that make walking very painful. If left untreated that fracture could develop into a complete break in the bone.
Stress fractures can be misleading to some because there is the misconception that they only occur from a slip, trip or fall but that is a myth. Athletes can get stress fractures from continuous weight bearing activities such as running, gymnastics and other sports. Others can develop stress fractures from simply standing on a hard floor too long. According to the American College of Foot and Ankle Surgeons, stress fractures can occur in a wide variety of seemingly minor circumstances like standing or walking for long periods of time. Some runners believethat since they can still walk on their foot there is no need to rest or reduce their activity level. “It can’t be broken, I can walk on it!” If someone continues to run or walk on it untreated; it could make the condition worse and the recovery prolonged.
It is important to recognize the signs of a stress fracture especially after a fall or stressful activity. Pain, swelling, redness and possibly bruising over the area can all be signs of a stress fracture. The symptoms usually improve with rest but come back once activity is resumed. If the pain continues after rest you want to follow the RICE protocol – Rest, Ice, Compression and Elevation.

If the pain and swelling last longer than a few days a visit to a podiatrist for an x-ray is needed. Treatment may include crutches, a surgical shoe or a cast or boot to immobilize the fracture. In some cases, surgery may be necessary if the stress fracture has progressed into a full fracture. Treatment can take 4 to 6 weeks IF you catch the problem early. Stress fractures can recur in some people especially in those who have fragile, soft bones. They can also occur in people with a certain foot type such as those with flat feet, high arched feet or long bones in their foot.
No matter if it is the first or third time you have a stress fracture, proper and early treatment is recommended, which includes allowing your foot to rest. If you suspect you may have a stress fracture please contact the team at Physicians Footcare so we can help you take the first step toward getting back to what you love to do.

Causes, Symptoms, and Treatment of Poor Blood Circulation in the Feet
Poor blood circulation in the feet and legs is often caused by peripheral artery disease (PAD), which is usually the result of a buildup of plaque in the arteries. Plaque buildup, or atherosclerosis, can be the result of excess calcium and cholesterol in the bloodstream. This restricts how much blood can flow through arteries. Reduced blood flow to a certain area of the body severely limits the amount of oxygen and nutrients that part of the body receives. This leads to degeneration in the muscles and other tissues. Sometimes, poor blood circulation in the feet and legs can be caused by other conditions, such as the damaging or inflammation of blood vessels, known as vasculitis.
The lack of oxygen and nutrients caused by poor blood circulation can restrict muscle growth and development, as well as cause muscle pain and cramps, weakness, and stiffness. Other common symptoms include numbness in the legs and feet, skin discoloration in the affected limbs, slower nail and hair growth, and erectile dysfunction in men. In more severe cases of PAD, pain can be present even when a person isn't exercising, and may range from mildly uncomfortable to completely debilitating.
Poor blood circulation in the feet and legs is more common in those who are overweight or obese, have diabetes, high blood pressure, high cholesterol, who smoke, or who have a family history of PAD or related conditions such as a heart attack, stroke, etc. Diabetes and smoking place a person at greatest risk for developing poor blood circulation, although advanced age, over 50, can also increase risk.
If you are experiencing poor blood circulation in the feet and legs caused by PAD, it is important to make changes to your lifestyle in order to reduce your risk of experiencing a heart attack or stroke caused by this condition. If you smoke, quit completely. This will increase the amount of oxygen in your bloodstream. Exercising and reducing the saturated fats in your diet. Saturated fats come from fatty meats, fried foods, whole milk, etc., can make a difference in improving blood circulation in feet. It is also important to avoid developing influenza and to carefully control your blood sugar if you have diabetes.
Your doctor may recommend combining lifestyle changes with a prescription medication regimen to improve blood circulation. The most commonly-used medications for PAD are called statins and work by blocking the amount of enzymes in your body that produce cholesterol. They are known by the brand names Zocor, Lipitor, Crestor, and others.
